It is a dermatophytic infection of the scalp. Tinea capitis in adults seems less in general. It can happen at all ages, especially in childhood. Tinea capitis hair loss is more common in boys than girls. Tinea capitis description is like this: The word tinea means the worm and the word capitis means the head. The causative agent of the disease is Trichophyton or Mikrosporum species. Anthropophilic dermatophytes grow with spores (endocervix) in the hair, and the hair comes to the position of broken at the level of the skin. Others involve ectocervix they multiply around the hair and disrupt the cuticle of the hair. So pale, broken hair occurs.
Tinea Capitis Types
There are 3 main clinical forms:
Tinea Capitis Superficialis (Ringworm)
Tinea capitis scalp, which is common in kindergarten and primary school children generally is not happening in adulthood due to the increase in some fungistatic fatty acids in the sebum that occurs with puberty. Existing infections usually disappear spontaneously after puberty.
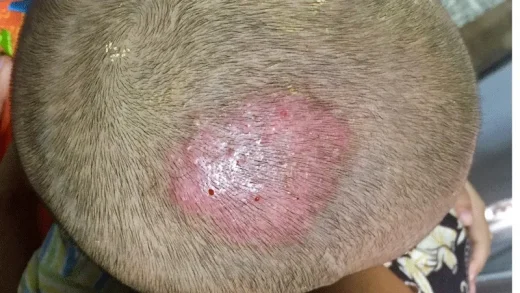
Tinea Capitis Profunda (Kerion Celsi)
This clinical form, which is the inflammatory form of tinea scalp, is a reaction happening by the body’s cellular immunity against fungal elements. Kerion cells, which appear before puberty, start as tinea capitis superficialis, then pustules and nodules of different sizes occur on the scalp, and a thick crust layer consisting of blood and pus forms on the lesion, which acquires a tumoral appearance. The hairs on the lesion stay loose and come off easily when pulled. It is like pulling a hair out of butter, pus comes from the follicles when pressed on. Patients may develop lymphadenopathy. Due to secondary infection, fever, and pain may occur in patients. Vesicular or pustular id reaction may occur from various parts of the body. Erythema nodosum may also become possible in patients. Lesions leave scars in their places.
Favus
Favus is a special form of scalp fungal disease. Infection, in which the causative agent is T. schöenlein, mainly affects the scalp, but can also affect the skin and nails. If a doctor would not treat the disease that starts before puberty, it can continue after puberty. The classic lesion of Favus is yellowish, sunken crusts located around the hair, called the scutula. It has an unpleasant odor (described as rat urine). There is an erythematous and atrophic floor under the scutula. It causes cicatricial alopecia, especially in the vertex. The scutula can fuse to form large plaques. During the healing process, tissue loss develops in the scalp, which causes permanent hair loss. It is not common nowadays.
Tinea Capitis Symptoms and Differential Diagnosis
Apart from clinical appearance, microscopy, and cultures can be used for diagnosis. Especially Wood’s light is important in the differential diagnosis.
It is important that the differential diagnosis of ringworms in hair. Such as; alopecia areata, pityriasis simplex, seborrheic dermatitis, psoriasis, tinea aminantecea, trichotillomania, secondary syphilis, impetigo, infected pediculosis capitis, kerion cells, DLE and lichen planus.
Tinea Capitis Treatment
Systemic antifungal drugs should be used. (To know about hair fungus, see: Hair Fungus) Itraconazole, terbinafine, fluconazole can be used in adults and griseofulvin in children.
As a tinea capitis treatment at home, shampoos containing selenium sulfide or ketoconazole can be used for it to stay on the ringworm on the head for 5 minutes. Meanwhile, materials such as brushes and combs used for protective purposes can be kept in this shampoo. Dandruff shampoos can increase the development of ringworm on the scalp.
To have more information about Tinea Capitis, please contact us to inform you!
Frequently Asked Questions
How can you get tinea capitis?
It generally spreads from the infected pillow, comb, or likewise.
How do you treat tinea capitis?
The most common treatment for tinea capitis is antifungal medications.
Does tinea capitis go away?
It is something that heals slowly. It generally loses its impact in 4-6 weeks.